Cryptorchidism
We call cryptorchidism when we can’t find the testicle in the scrotum.
It is the result of an incomplete descent of the testicle from the abdomen until the scrotum during fetal life. Formed in the abdomen, the testicle follows a pathway through the groin and into the scrotum during the last weeks of gestation.
Almost 95% of cases show a palpable testicle in the groin area. Usually, the diagnosis is made immediately after birth during the routine medical examination in the maternity ward. Ultrasound examination is not mandatory when the testicle is palpated in the physical exam.
The undescended testicle can improve in the first months of life or go on unchanged. A re-examination at 6 months of age is necessary for confirming the diagnosis and establishing the surgical assessment if needed. In the condition of no palpable testicle, laparoscopy is indicated as an unequivocal diagnostic tool and as surgical therapy.
Inguinal hernia can be associated with cryptorchidism. Premature infants are more at risk of developing cryptorchidism.
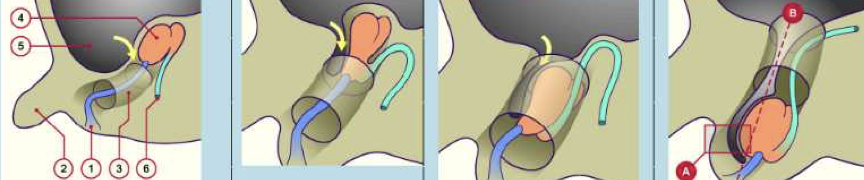
ORCHIPEXY
Surgery for bringing the testicle to its normal location in the scrotum is named orchipexy. Surgical treatment is required for two important reasons: an undescended testicle is subject to a higher body temperature which results in decreased sperm production and subsequently infertile and, an intra-abdominal testicle has a higher risk for developing cancer. For best results, the operation should be performed before your child turn 1 year of age. Depending on where the testicle is located, this may be done as a "day clinic" operation under general anesthesia.